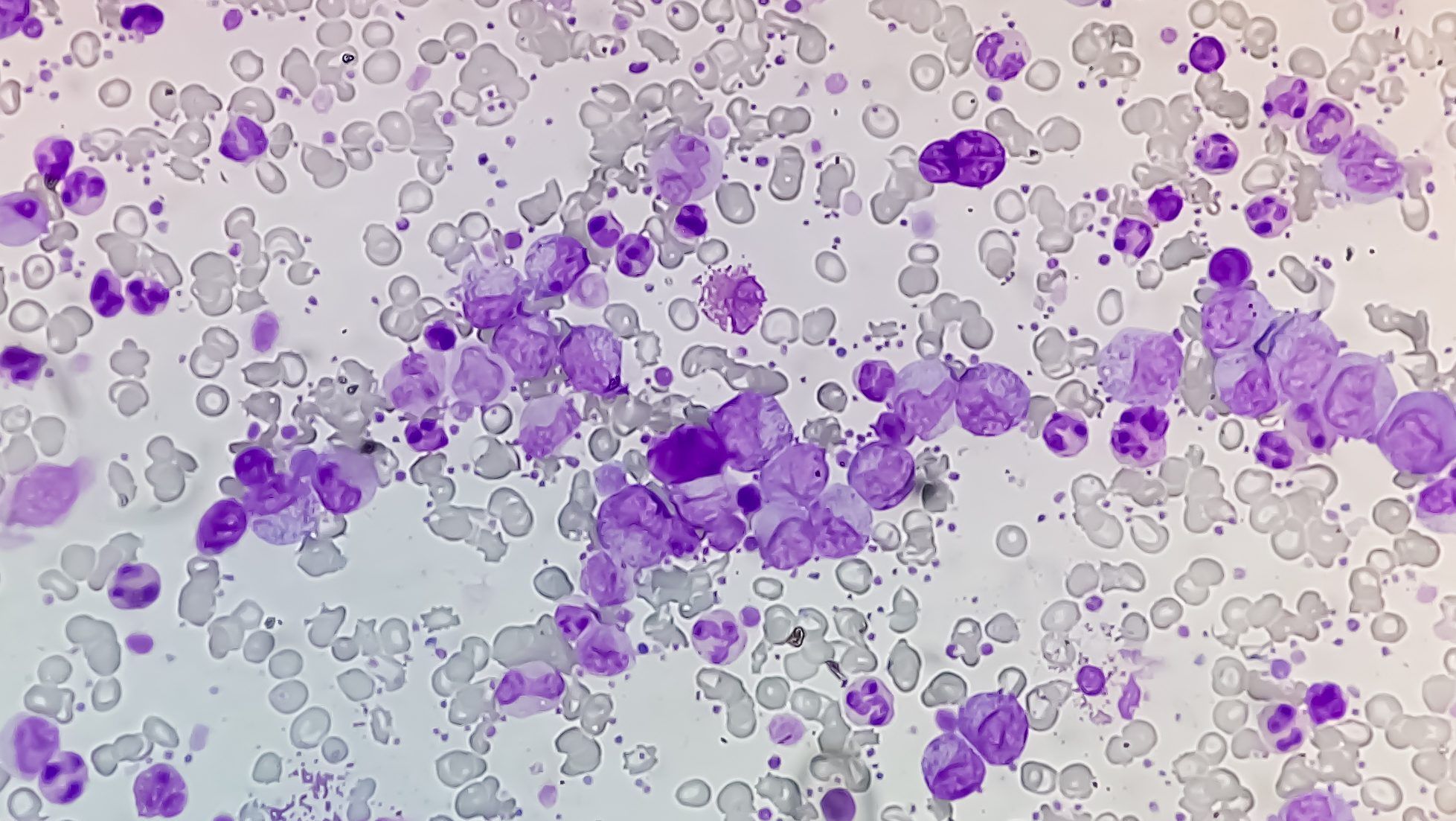
essential thrombocythemia: how a racing heart led to a rare blood cancer diagnosis
in the years leading up to her diagnosis, janet pieschel experienced other symptoms like light-headedness and excruciating migraines.
rare diseases: 'it's difficult to get the government to understand the importance of adopting new drugs'
john clark, who lives with polycythemia vera, a myeloproliferative neoplasm (mpn), says one of the biggest challenges for people with an mpn is access to medication. his treatment costs $60k per year.
'an old person's disease': how did stomach upset turn out to be a rare blood cancer?
carol cameron was 39 when she was diagnosed with essential thrombocythemia, a rare blood cancer that typically affects people over the age of 60.
 5 minute read
5 minute read