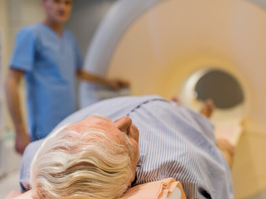
patients living with advanced skin cancer have treatment options available
top oncologist advises patients with cutaneous squamous cell carcinoma to be proactive in their care and ask health-care providers about options

since dave sutherland was diagnosed with cutaneous squamous cell carcinoma in 2007, he’s become increasingly involved in his own care plan. photos: mike drew

this story is sponsored by
a research-based pharmaceutical company
this story was created by content works, postmedia’s commercial content division, on behalf of a client.
when dave sutherland learned in 2007 that he had cutaneous squamous cell carcinoma, it came as a huge shock. not only because he was just 36 years old at the time, but also because three years earlier he had been told by a gp the patch of red, scaly skin on his right shoulder was eczema. since then, sutherland and his family have struggled to come to terms with the diagnosis. “my cancer has had a huge impact on my family and my career. one of the hardest things i had to do was tell my kids that i’m not going to survive this. i also had to drop out of my degree program and be away from home for up to six weeks while receiving treatment.”
cutaneous squamous cell carcinoma (cscc) makes up 20 per cent of all skin cancers and affects one in 20 canadians. this means there are approximately 17,500 people in canada like sutherland living with this type of skin cancer.
according to dr. alex mlynarek, surgical oncologist at mcgill university, cscc is usually caused by sun exposure — typically in the head and neck region. “a lot of my patients have a history of being out in the sun without sunscreen,” he says. “the ultraviolet rays damage the skin which, over time, can cause the skin cells to become cancerous.”
dr. mlynarek is seeing rising cases of cscc among the elderly, though it can arise in younger canadians too. “seniors are more likely to have a suppressed immune system, and many didn’t use sunscreen when they were growing up,” he explains.
advertisement

“you have to live your life as best you can,” says sutherland, seen here with his canine companion, buster.
cutaneous squamous cell carcinoma (cscc) differs from melanoma — a less common form of skin cancer
— in several ways. whereas melanoma affects melanocytes, cells located in the lower layer of the skin, cscc affects squamous cells, which are close to the surface of the skin.
“top oncologist says he sees better physical and psychological outcomes among patients who are involved in their own care.”
“typically, melanoma is a more aggressive type of cancer than squamous cell and is more likely to spread,” explains dr. mlynarek. “but when cutaneous squamous cell carcinomas spread, they are much more visible and tend to invade nearby structures, such as the ears, eyes and neck.” at this point, cancerous skin patches aren’t just thickened, dry, or itchy — they can be disfiguring, dangerous, and even deadly.
once cscc has spread locally, it can attack internal organs, such as the lungs, liver, and brain.
this is precisely what happened to sutherland. after his initial treatment in 2007, his cancer returned in 2009 and had spread to his lymph nodes, making it stage 3. today, sutherland has stage-4 cscc, as the cancer spread to his brain in 2017. “i’m now partially blind, unable to work, suffer from headaches and dizziness,” he says. “i’ve lost a lot of freedom because i can no longer drive.
advertisement
when first diagnosed, sutherland blamed himself for not catching it sooner. “i was angry at myself because i didn’t push to see a dermatologist when the cancer first showed,” he recalls. after his diagnosis in 2007, sutherland describes those first few years as a constant worry over treatments and time away from his family.
categories accessible to canadians:
- surgery (the physical removal of cancerous tissue)
- radiation (shrinks the tumour using targeted high-energy particles)
- immuno-oncology (shrinks the tumour by helping your immune system fight your cancer). this category has been issued marketing authorization with conditions, pending the results of trials to verify clinical benefit.

despite the challenges of his illness, sutherland tries to focus on the positives in his life, such as regular walks with buster.
sutherland is also an advocate for cscc patients getting more involved in their care plan and learning as much as they can about the resources available for support. “don’t be afraid to ask questions and get a second opinion,” he advises. “a referral or treatment may not be offered unless you ask for it. be persistent and trust your medical team to support you.”
advertisement
sutherland encourages anyone facing cscc to take control of their own health care as best they can. “one thing i always recommend to people is to be your own advocate,” he says. “if i had asked for a dermatology referral when i was concerned, it would have saved me a lot of grief.”
despite the challenges of his illness, sutherland tries not to dwell on the negative. “you have to live your life as best you can,” he says.
dr. mlynarek says he’s seen better physical and psychological outcomes among those who are more informed and involved in their care, compared to those who do not play an active role in their health. “i like to include patients and their families in the decision-making process, so they can consider a variety of options. it’s imperative they understand what’s happening to them and what it involves.”
all treatment options have benefits and risks that vary by individual. patients should consult their health-care provider to determine the most appropriate option. to learn more about cscc and help prepare for your next medical check-up, visit melanoma canada.
this story was created by content works, healthing.ca’s commercial content division, on behalf of a research-based pharmaceutical company.
 4 minute read
4 minute read