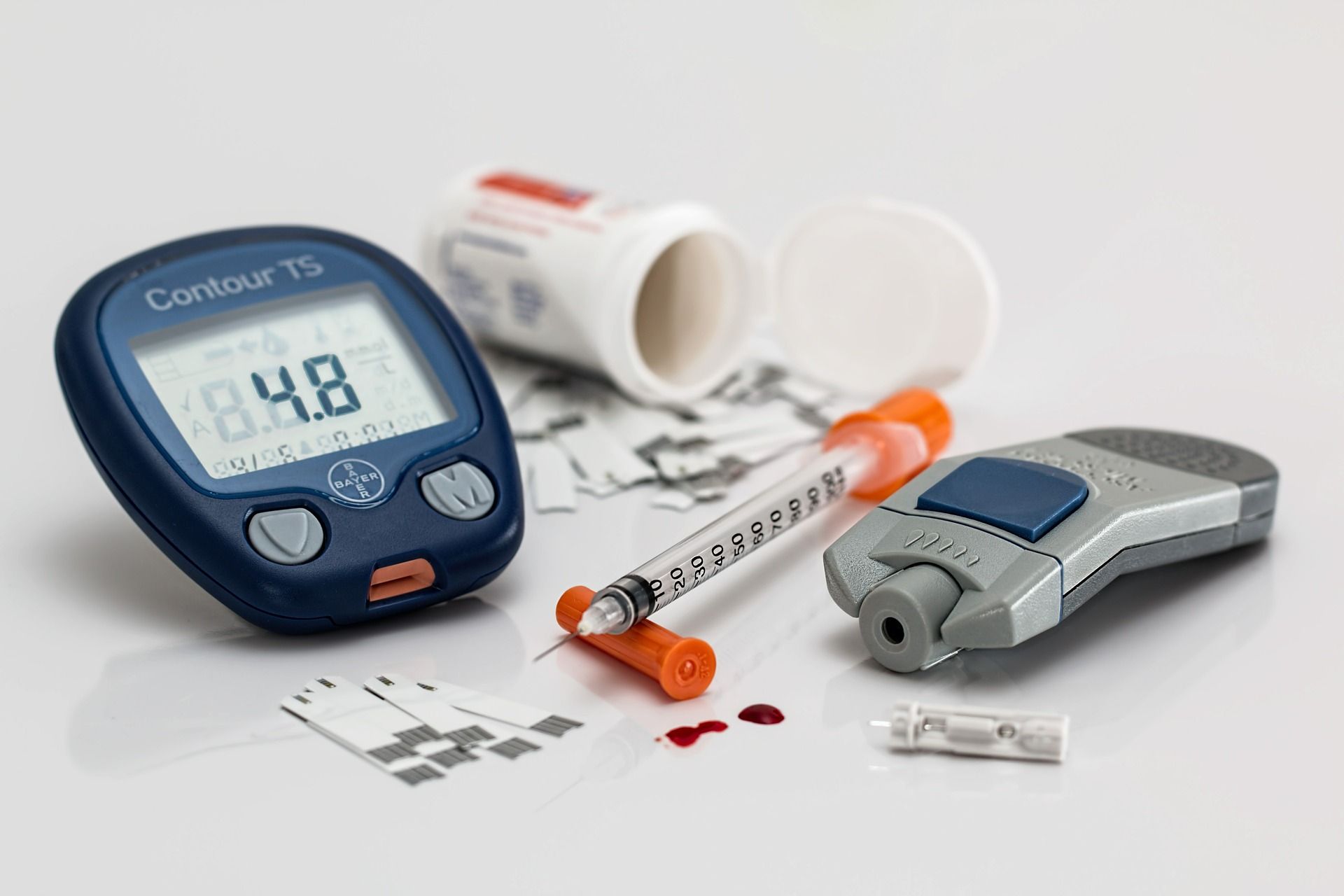
lean diabetes is rare, affecting about two per cent of people with type 2 diabetes
when someone lean is diagnosed with type 2 diabetes, they may be at an increased risk for vision and nerve damage, poor blood circulation, kidney and heart disease.
what are the signs of hypoglycemia?
the most common symptoms of low blood sugar include trembling, sweating, anxiety, confusion, nausea or difficulty concentrating.
what it feels like: type 2 diabetes is 'not something to hide and keep away from people'
nicole cleaver talks about her experience with diabetes, managing the highs and lows, and why she's grateful for the invention of insulin.
 6 minute read
6 minute read