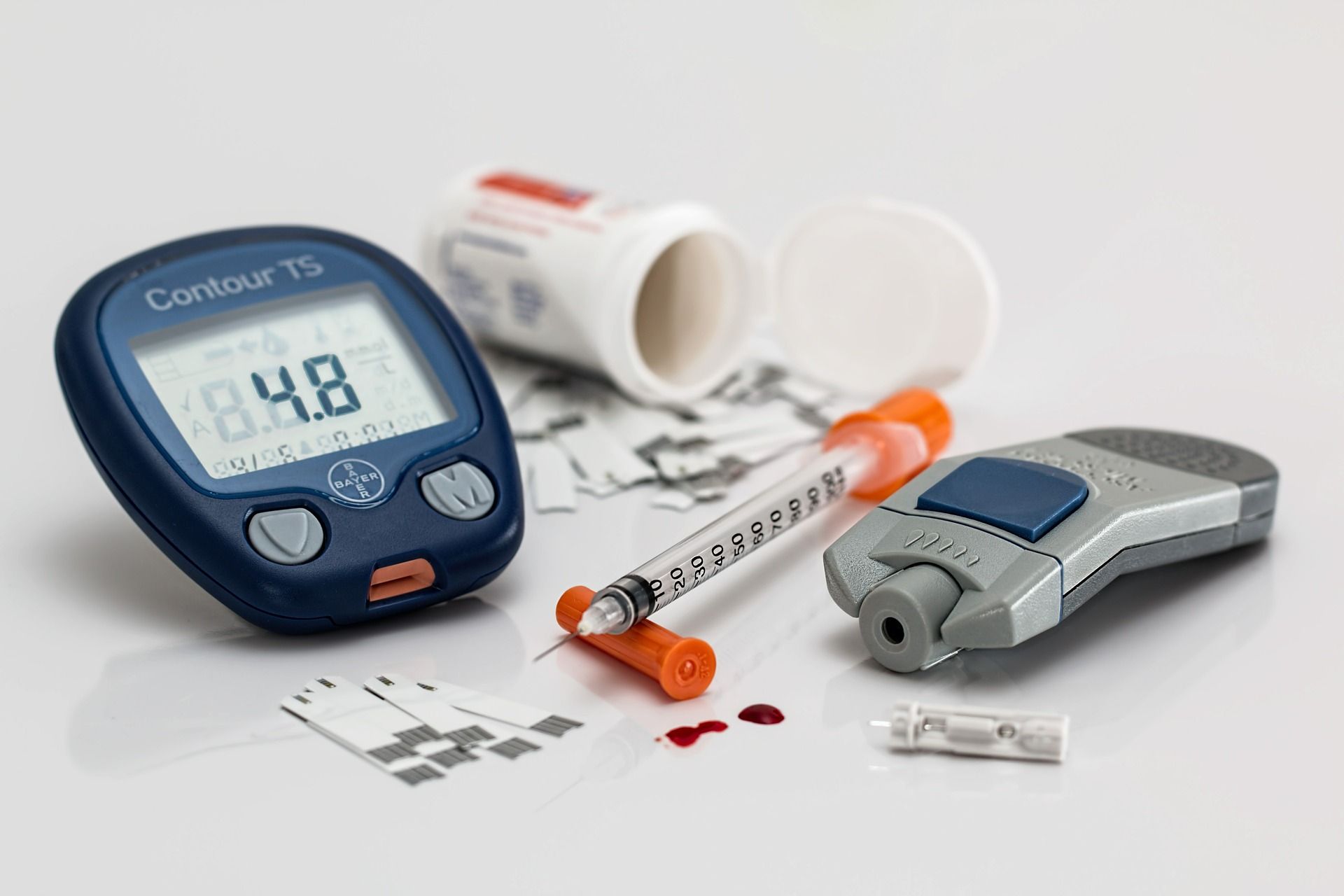
opinion: it's more cost-effective for governments to cover diabetes technology, plus it saves lives. so why aren't we doing it?
all patients with type 1 diabetes should have access to the advanced glucose monitors and insulin pumps that improve health outcomes and reduce complications, hospitalizations, and the risk of death.
diabetes and blindness: 'when you are in your twenties, you think you're invincible'
for ryan hooey, the first sign that he had diabetic retinopathy, the symptoms of which include blurry vision and floaters, was darkness.
lean diabetes is rare, affecting about two per cent of people with type 2 diabetes
when someone lean is diagnosed with type 2 diabetes, they may be at an increased risk for vision and nerve damage, poor blood circulation, kidney and heart disease.
 6 minute read
6 minute read