getting manitoba, ontario, and québec back on track would save 170 lives, the report estimates. it would also save the provinces $122.6 million in direct medical costs, but would require 540, 7,700, and 2,800 annual treatments, respectively.
“the ministry of health funds 18 multidisciplinary hepatitis c care and treatment teams located in community and health organizations across ontario,” reads a statement provided by the ontario ministry of health. “these teams work with people who are at highest risk of acquiring hepatitis c and who face systemic barriers to accessing mainstream health and social services.
“ontarians can also access hepatitis c testing, care and treatment through primary care, hospital and community-based specialists and other health care models, such as ontario health teams.”
feld adds the teams set up to eliminate hepatitis c are working hard to reach remote and marginalized communities, key to reaching these goals. as the liver is also fairly resilient, once a patient gets access to treatment for viral hepatitis c, the prognosis is often quite good.
why is ontario having trouble reaching hepatitis elimination goals?
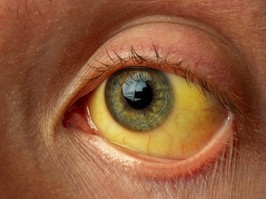
hepatitis c may not cause symptoms for years, meaning unknown transmission of the virus is one of the greatest threats to elimination targets.
 3 minute read
3 minute read