non-invasive brain stimulation provides promise for treatment of depression and anxiety
transcranial magnetic stimulation (rtms) delivers magnetic pulses on the outside of the skull to modulate the brain’s circuitry to target the area of the brain that would respond to therapy.

preliminary studies on the impact of transcranial magnetic stimulation on patients are showing positive outcomes.
getty
for years, interior designer raija hilska felt like she was “always dragging something along.” deep melancholy, profound sadness, raw emotions and, sometimes, thoughts of suicide. for long periods, she was unable to work.
“i would always say ‘i can’t trust tomorrow,” she says. “who knows what my mood will be?’”
diagnosed with bipolar disorder in 2003, raija has been under the care of a psychiatrist at the royal ottawa mental health centre (the royal), and while lithium and other drugs provided some relief over the years, life became especially dark during the lengthy covid-19 pandemic. “i was quite depressed, quite suicidal,” says the finnish-born mother of two and grandmother of three. “over the years, i’ve tried all kinds of different medications. i felt that there had to be another solution.”
and then she found it.
raija was referred to a study at the royal that uses repetitive transcranial magnetic stimulation (rtms) — a non-invasive therapy that delivers magnetic pulses on the outside of the skull to modulate the brain’s circuitry.
thanks to brain canada funding, a preliminary rtms study mapped the brains of 16 healthy controls by measuring cellular activity and brain circuitry to target the area of the brain that would respond to therapy. a subsequent study tested rtms on 22 people living with depression and anxiety. a larger study, which aims to recruit 200 people, is now underway.
advertisement
within a week of starting daily three-minute doses of rtms in a hospital clinic, raija started “feeling different for the first time ever, i felt like my eyes had opened.”
for the next four weeks, daily treatment – pulses delivered via a small paddle that emits a tapping sound – continued. then, treatments shifted to weekly sessions.
as part of the study, raija filled out lots of questionnaires, answered questions after every session, had follow-up phone calls from researchers, and underwent further assessment. she also continued to take her prescribed medications.
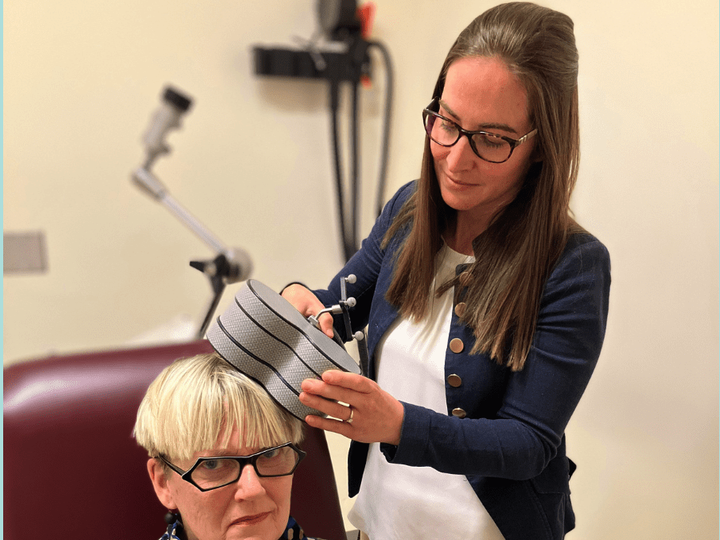
within a week of starting daily three-minute doses of rtms, raija hilska says she “started feeling different for the first time ever. i felt like my eyes had opened.”
when the darkness lifted, raija couldn’t believe it.
“this research has helped me,” says raija, after seven weeks in a rtms study. “when you’re not feeling well, you tend to dwell on things. when you are able to control your brain, your thinking is more compact, and you are able to focus. i don’t look back as much as i used to.”
she hopes that brain canada-funded research at the royal will one day help make this relatively low-cost and non-invasive therapy (first approved by health canada for the treatment of depression in 2002) accessible and part of standard care for mood disorders, which affect as many as one in three canadians in their lifetime. the therapy is not covered by most provincial health insurance plans.
advertisement
so far, neuropsychologist and neuroscientist dr. sara tremblay of the royal says outcomes have been excellent, with a high percentage of study participants responding positively to treatment. her first two studies on the therapy are expected to be published this fall.
“my family was curious about what it (rtms) was like, what it felt like,” raija says. “i told them it’s like getting your highlights done.”
that’s not to say that there are no side effects. initially, she had some headaches and felt fatigued, but those symptoms, which eventually went away, are also characteristic of depression.
“i told the therapists who deliver the treatment that i was worried,” she says. “they said ‘what’s wrong?’ and i told them i’m feeling so normal. and we all laughed.”
she also worried that brain stimulation would tip her into mania, but that hasn’t happened. and though she is concerned that she could backslide, raija feels reassured knowing the therapy worked once and would probably work again, if needed.
for now, she says she plans to “live for today.”
learn more about transcranial magnetic stimulation (rtms).
 3 minute read
3 minute read





